Clindamycin and Clostridium Difficile, how are the two related and how to avoid CDAD
What is the risk of clostridium difficile when taking Clindamycin?
The use of Clindamycin, like many other antibiotics, can lead to an overgrowth of the bacterium Clostridium difficile, which can cause a serious infection known as Clostridium difficile-associated diarrhea (CDAD).
C. difficile is a naturally occurring bacterium in the gut of many people, but when antibiotics such as Clindamycin are taken, they can kill off the beneficial bacteria that normally keep C. difficile in check, allowing it to grow and produce toxins that cause diarrhea and inflammation in the colon.
The risk of developing CDAD when taking Clindamycin is increased, especially in elderly individuals, those with weakened immune systems, and people who have had previous episodes of CDAD. It is important to note that not everyone who takes Clindamycin will develop CDAD, but if you experience symptoms of diarrhea, fever, abdominal pain, or blood in your stool while taking Clindamycin or even after stopping the medication, you should contact your healthcare provider immediately.
Your healthcare provider may order a stool test to check for the presence of C. difficile or other causes of diarrhea, and may also consider stopping or changing your antibiotic treatment if it is deemed necessary. Additionally, taking probiotics or other medications to restore the balance of beneficial bacteria in your gut may help reduce your risk of developing CDAD while taking Clindamycin.
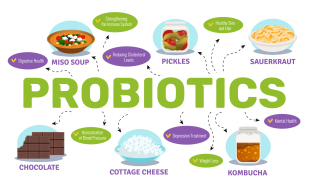
How effective are probiotics when taking antibiotics?
Probiotics have been shown to be somewhat effective in reducing the risk of Clostridium difficile-associated diarrhea (CDAD) and other antibiotic-associated side effects when taken alongside antibiotics. Antibiotics can disrupt the balance of bacteria in the gut, killing off not only harmful bacteria but also beneficial ones that help maintain healthy digestive function. Probiotics are live microorganisms that can restore the balance of bacteria in the gut, potentially reducing the risk of CDAD and other antibiotic-associated side effects. Research suggests that taking probiotics alongside antibiotics may reduce the risk of developing CDAD by up to 60%. However, not all probiotics are equally effective, and the strains and doses that are most effective may vary depending on the individual and the specific antibiotic being taken.
It's important to note that while probiotics may help reduce the risk of CDAD and other antibiotic-associated side effects, they should not be viewed as a substitute for medical treatment. If you experience any symptoms while taking antibiotics, such as diarrhea, fever, abdominal pain, or blood in your stool, you should contact your healthcare provider immediately. Additionally, you should talk to your healthcare provider before starting any probiotic supplement to ensure that it is safe and appropriate for your individual needs.
Should probiotics be taken simultaneously with antibiotics? Or should they be taken separately?
One might thing to take probiotics at the same time as antibiotics, as this may seem logical and certainly more convenient. The reality is that most antibiotics at the pharmacy today are very
effective at neutralizing the target bacteria, but can also really upset the normal flora in our guts. This idea also affects the probiotic. Dr Estafan recommends taking the probiotic between doses
of the antibiotic, and preferably with food. This enables the probiotic to bind with the food and make its way down to the lower GI where it is needed the most. If the antibiotic and probiotic are
taken at the same time, the antibiotic wipes out much of the benefit of the probiotic. Dr Estafan describes how to take a probiotic (in this case with a different antibiotic, amoxicillin) in this video.
Some probiotics are more heat-sensitive and may be destroyed by antibiotics, so it is important to check the label or consult with a healthcare provider to determine the appropriate timing for taking probiotics with antibiotics. Some studies suggest that taking probiotics at least 2 hours before or after antibiotics may help to maximize their effectiveness, while others suggest that taking them together may be equally effective.
Additionally, the type of probiotic strain being used may also influence the timing of supplementation. For example, some strains of probiotics may be more effective when taken with meals, while others may be more effective when taken on an empty stomach.
Overall, it's important to follow the instructions on the label of the probiotic product or to consult with a healthcare provider to determine the appropriate timing for taking probiotics alongside antibiotics.
What are the guidelines for antibiotic prophylaxis for dental cleanings?
Antibiotic prophylaxis, also known as antibiotic premedication, is the use of antibiotics before a dental procedure to prevent infective endocarditis (IE) in patients who are at risk. The guidelines
for antibiotic prophylaxis for dental cleanings vary depending on the patient's medical history and individual risk factors.
According to the American Heart Association (AHA) guidelines updated in 2017, antibiotic prophylaxis is not recommended for most patients undergoing dental procedures, including dental cleanings. The AHA guidelines suggest that the use of antibiotics before dental procedures should be reserved only for patients at highest risk of IE, including those with:
- Artificial heart valves
- History of IE
- Certain congenital (present from birth) heart conditions, such as unrepaired or incompletely repaired cyanotic congenital heart disease, a completely repaired congenital heart defect with prosthetic material or device, and certain types of surgically constructed shunts or conduits.
For these high-risk patients, the AHA guidelines recommend a single dose of an appropriate antibiotic taken orally, 30 to 60 minutes before the dental procedure.
It is important to note that the use of antibiotic prophylaxis should be based on an individualized assessment of the patient's risk factors and medical history, and should be determined in consultation with a healthcare provider. Patients should always inform their dentist and healthcare provider of any heart conditions or other medical issues before undergoing dental procedures.
Are antibiotics necessary before dental cleanings for people with prosthetic joints?
The American Dental Association (ADA) and the American Academy of Orthopedic Surgeons (AAOS) do not recommend routine antibiotic prophylaxis before dental cleanings or other dental procedures for patients with prosthetic joint replacements.
According to the ADA/AAOS clinical practice guideline released in 2013, the use of antibiotics before dental procedures should be limited to patients with the highest risk of developing a prosthetic joint infection (PJI), including those with:
- A history of previous PJI
- Immunosuppression
- Inflammatory arthritis
- Malnourishment
- Hemophilia
For patients without these risk factors, antibiotic prophylaxis is not recommended before dental cleanings or other dental procedures.
It is important to note that the decision to use antibiotic prophylaxis should be based on an individualized assessment of the patient's risk factors and medical history, and should be made in consultation with a healthcare provider. Patients with prosthetic joints should always inform their dentist and orthopedic surgeon of their joint replacement and any other medical issues before undergoing dental procedures.